Ticks: Hold the Line
Infectious diseases transmitted by ixodid ticks present a serious problem in many countries worldwide. In Russia, ticks bite about half a million people every year, and more than two thousands of those bitten by ticks contract tick-borne encephalitis, a serious viral disease causing damage to the nervous system, sometimes leading to death. Tick-borne infections pose threat to everyone who spends much time in nature: timber cutters and geologists, hunters and fishermen, villagers and seasonal gardeners, hikers and campers, even people who like to take walks. This article, which continues a series of publications on ixodid ticks as disease carriers, describes the risks for humans to become victims of these blood-sucking arthropods and shows how to protect against them. This information will be useful to everyone who wants to protect themselves and their loved ones from this very real danger
Before we talk about measures to protect against ixodid ticks, we wish to recall the most important facts about the lifestyle of these arthropods. By the way, ticks are often mistakenly called insects, but one can easily tell a possible parasite from a harmless bug by the number of legs: adult ticks have eight legs like spiders, their distant relatives in the class of arachnids, instead of six ones like insects.

The life cycle of ixodid ticks includes three stages, not counting the egg: the larva (six-legged!), the nymph, and the adult (imago). At each stage in its development, the tick must at least once suck in enough blood, with the larva, nymph, and imago usually feeding on different animal hosts.
Many potential “victims” of ticks, primarily small rodents, are natural reservoirs of the so-called zoonotic infections. Therefore, at each stage in its life, the tick interacts with the blood of the animal host and can either receive the causative agents of these infections or, conversely, infect the host through the secret of its salivary glands. Although ixodid ticks as “bloodsuckers” do not pose any significant threat to humans, their bites can transmit pathogenic viruses and bacteria that are dangerous to humans.

It is not only the long-sucking adult females that act as carriers of pathogens. Males, needing much smaller volumes of blood, as well as the barely noticeable small nymphs, can too carry disease. By the way, one can catch the virus of tick-borne encephalitis even by drinking raw milk of goats on which infected ticks have fed.
In our middle latitudes, ixodid ticks usually “go hunting” in the period from March to April. A chance of meeting them arises on the first warm days when the daytime temperature reaches 4–5 °C. Of course, the most effective measure to protect against ticks is to spend as little time as possible in hazardous areas, but our warm season is already too short. Therefore, one must learn how to use—properly and effectively—protective clothing and apply chemical protective products. Moreover, when visiting possible ticks’ habitats, one must do regular checkups and quickly remove attached ticks to prevent transmission of infectious agents.
The tips below will help all nature lovers to get fully prepared for the tick activity season.
Ticks go hunting
 These arthropods need high humidity, so they hide in forest litter, thick grass, and even in household waste. Therefore, gardeners are advised to remove, every autumn, foliage and dry grass, in which ticks can overwinter.
These arthropods need high humidity, so they hide in forest litter, thick grass, and even in household waste. Therefore, gardeners are advised to remove, every autumn, foliage and dry grass, in which ticks can overwinter.
Ticks prefer such habitats as forest glades overgrown with fern and moss, forest edges turning into a meadow, ravines with streams, and slopes covered with tall grass and small trees. All these places are inhabited by animals on which ticks feed: small rodents (field voles, mice, squirrels), hares, ungulates, etc. Ticks can occur not only in deciduous forests with rich grass but also in coniferous ones, where they hide in brushwood piles, which are fancied by small forest animals.
Contrary to popular belief, ticks do not attack people from trees. Hungry individuals climb up grass blades and bushes, where they sit and wait for potential hosts to pass by. Thus, people should beware of the sides of forest roads, covered with vegetation, which may pose significant danger—one should keep away from tall grass and stick to the middle of the road.
The most common disease transmitted by ixodid ticks in the temperate latitudes of Eurasia is ixodid tick-borne borreliosis (Lyme disease), which is caused by a whole group of bacteria of related species from the Borrelia burgdorferi complex (Korenberg et al., 2013). This is a multisystem disease with a wide range of skin, articular, neurological, and cardiovascular manifestations; a presenting feature in the early stages is migratory erythema. Ticks can also transmit another type of borrelia, B. miyamotoi, which is genetically close to the pathogens of tick-borne relapsing fever. This disease was first described on the territory of Russia (Platonov et al., 2011). Unlike Lyme borreliosis, it occurs in a febrile form without the development of erythema. Modern test systems do not provide reliable diagnosis of borrelioses, and in the absence of erythema, it is difficult to diagnose the disease.
An important group of bacterial infections transmitted by ticks are rickettsioses, which are caused by intracellular parasitic bacteria.
In the European part of Russia, Astrakhan spotted fever has been reported, which is caused by the Caspian subspecies of Rickettsia conorii, which is transmitted by Rhipicephalus pumilio ticks (Rudakov, 2016). In Siberia, there have been cases of Siberian tick-borne typhus whose causative agent is R. sibirica, and in the Far East, rickettsiosis is most often caused by R. heilongjiangensis (Mediannikov et al., 2004). Recently, cases of rickettsioses with atypical symptoms, i. e., with the absence of a characteristic rash, have been reported in Western Siberia. It turns out that these infections were caused by R. raoultii, a widespread species of rickettsia, previously considered nonpathogenic, and by R. helvetica (Igolkina et al., 2018).
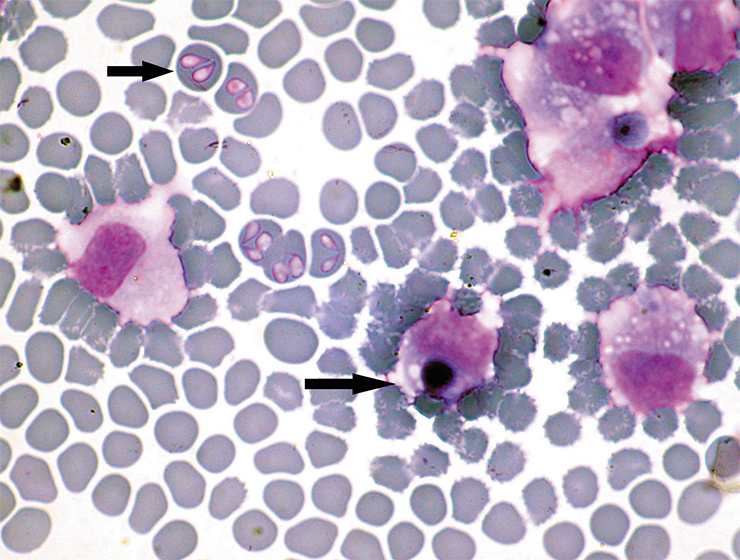
Ixodid ticks also act as carriers of protozoan hemoparasites of the genera Babesia and Theileria. In humans, babesias cause acute infections, including lethal ones. In Russia, there have been no cases of babesiosis in humans, but severe babesioses and theilerioses often occur in domestic and farm animals (primarily in dogs and horses)
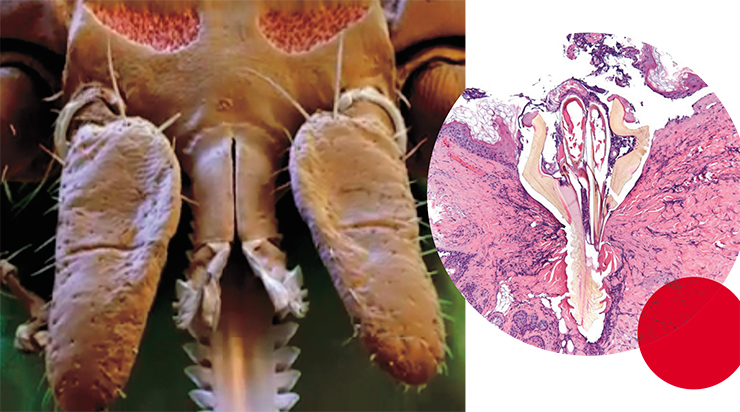
Ticks detect a possible host using their Haller’s organ, with which they perceive changes in carbon dioxide concentrations, specific odor components, and thermal radiation at a distance of up to 10 m. Most ticks attach to people’s legs and then crawl up the body in search of a place for suction. Therefore, it is recommended for those taking a walk in the woods to conduct mutual or self-checkups every half hour to remove possible ticks.
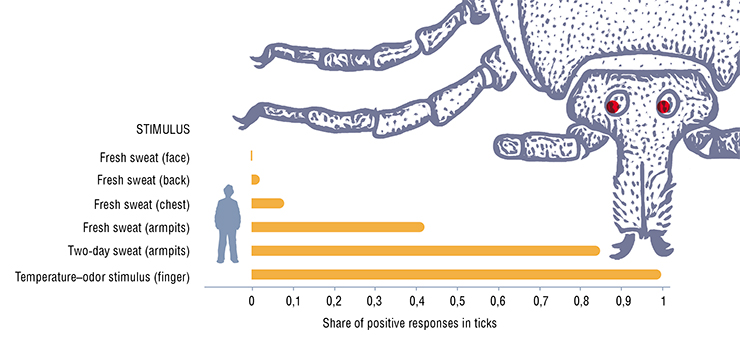
 Which people are most attractive to ticks? Experts from the Novosibirsk Institute of Animal Systematics and Ecology SB RAS have shown in experimental studies that although ticks find the smells of women more attractive, it is men who collect more ticks. The reason is that men sweat more and emit more heat and carbon dioxide and, thus, present a more visible target for ticks, which therefore attack them more often.
Which people are most attractive to ticks? Experts from the Novosibirsk Institute of Animal Systematics and Ecology SB RAS have shown in experimental studies that although ticks find the smells of women more attractive, it is men who collect more ticks. The reason is that men sweat more and emit more heat and carbon dioxide and, thus, present a more visible target for ticks, which therefore attack them more often.
Children 5–13 years of age also run a high risk of a tick bite as they spend a lot of time outdoors. When choosing a place for children’s games, one should avoid areas with thick grass and bushes.
Ticks are capable of penetrating to the victim’s body through a variety of barriers—experience shows that neither special clothing nor repellents can guarantee 100 % protection. Tick can hide in clothes, in a sleeping bag, or in other camping gear and attack a person after returning from the forest. Depending on humidity, they can survive in people’s homes for many days. Therefore, when you come back home, you should carefully examine yourself and your children and pets and thoroughly check all the clothes. It is advisable to wash the latter in hot water and then dry or iron. Ticks can survive washing at 40 °C, but they die at 65° and in the dryer.
Protective armor
The common means of protection against ticks are repellents, which keep away these arthropods, and acaricidal drugs, which kill them. One should always remember that ticks are not insects and many protective agents that work against mosquitoes and midges will not be as effective against ticks.
Effective protection against ticks comes from repellents based on DEET, a broad-spectrum substance, which may be applied onto the skin. The effectiveness of the repellent depends on the concentration of the active principle, on air temperature and wind strength, and on the level of perspiration.

Recent studies have shown that DEET, like several other repellents, disrupts the functions of Haller’s organ. Normally, ticks are able to detect the location of a human at a distance of several meters by his/her infrared radiation using a special spherical structure with a hole in its front part. DEET-type repellents interfere with the functioning of this infrared homing device (Carr & Salgado, 2019).
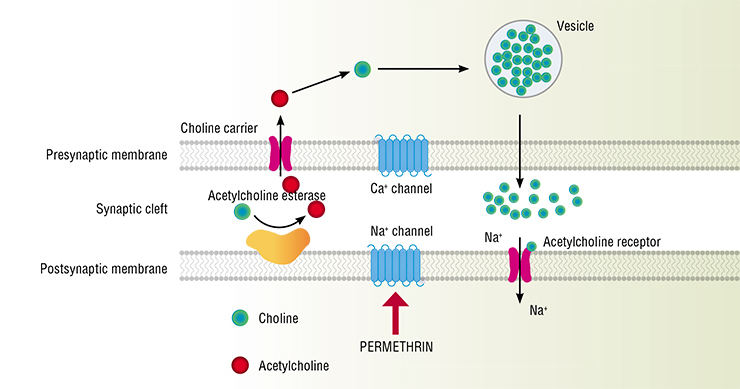
Acaricidal drugs include pyrethrins, natural insecticides contained in the flowers of some perennial plants of the Asteraceae family, such as the once famous Persian (or Dalmatian) chamomile. Natural pyrethrins are unstable in the light, and although they can quickly paralyze the arthropods, many of the affected individuals can cope with the toxin and survive. Therefore, pyrethrins are often combined with substances such as piperonyl butoxide, which inhibits the enzymes that break them down.
Today, acaricidal drugs are produced on the basis of pyrethroids, i. e., synthetic, chemically modified analogues of pyrethrins. These compounds, especially those of the second and third generation, are less volatile and more stable in the light than the natural ones and also have a higher anti-tick activity.
Pesticides are usually sprayed in early spring. As a rule, they are used at resorts and children camps, in parks and forest plots in cities, and at cemeteries. The most common products against ixodid ticks are those based on synthetic pyrethroids, such as Tsifoksa, Taran, and Baiteks. The Super Sipaz product can be used to kill tick larvae as well as adult ixodid ticks
Like pyrethrins, all pyrethroids are very toxic to fish and other aquatic organisms but are generally not so harmful to mammals and birds. Pyrethroids, which are effective against ticks, exert a paralyzing effect on the latter; i. e., ticks fall off the treated clothes and die.
Pyrethroid-based chemicals are usually available in the form of aerosols, which must not be applied directly onto the skin; they may be used only on clothes and only in the open air. It is recommended to perform the treatment in advance, i. e., slightly moisten the clothes with the aerosol and then dry them in the air before putting them on. Once applied, the substance remains effective for a long time; therefore, the treatment should be repeated no more than once every two weeks.
In Russia, pyrethroid-based means of personal protection against ticks include aerosols of various brands, such as Picnic, Tornado, Gardex, Permanon, Fumitoks, Briz, Komaroff, etc.; Reftamide-Taiga; Pretix (in the form of a chalk bar). Also, there are products that contain two different active substances, including DEET, e. g., the Kra-Rep and Moskitol-Antikleshch aerosols. When used properly, these products provide the maximum effect.
The market also offers a broad range of anti-tick remedies with unproven effectiveness. For example, products based on essential oils do provide short-term protection against mosquitoes and midges, but there is no evidence of their anti-tick activity. The widely advertised ultrasound devices do not scare ticks away either. Even DEET-impregnated bracelets can only prevent ticks from crawling along the arm or leg, and they work only if they fit snugly on the limb.
There are even more ridiculous recommendations. For example, it is said that anti-tick protection can come from eating garlic and other odorous products, up to whiskey and home-distilled liquor. However, these beliefs do not stand up to scientific rigor. The same concerns tips like putting one’s outerwear for a few minutes on an anthill or covering them with ash from fire. Perhaps, if all the clothes are sprayed with an acrid-smelling liquid, such as formic or acetic acid, then ticks will not like it (and neither will humans). However, the protective effect will unlikely be strong and lasting.
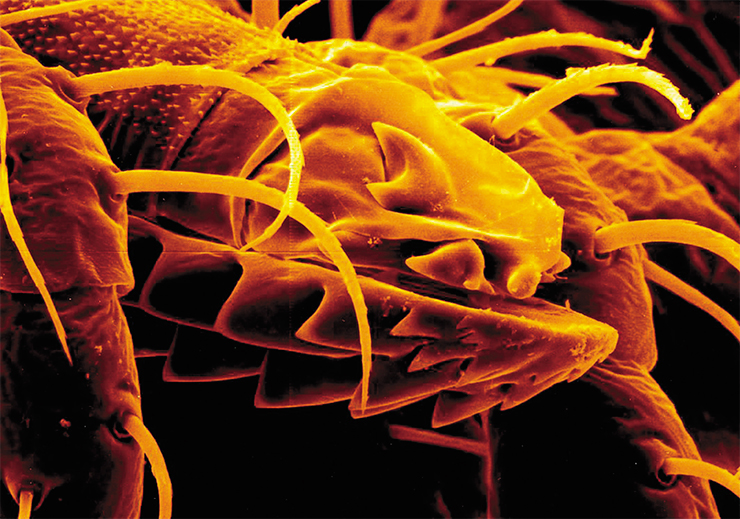
Admittedly, even the best anti-tick agents will not provide 100 % protection. To begin with, it is hardly possible to apply them over the entire surface of the body while ticks are real geniuses in overcoming obstacles. Practice shows that one can find a tick unexpectedly anywhere on the body. Moreover, since tick bites are usually painless (along with saliva, ticks inject anesthetics under the skin), one needs to conduct a thorough check of the entire body to detect a sucking tick.
What to do after a tick bite?
So, you have found a tick on yourself. What should you do? Do not try to crush the removed tick with your hands because viruses and other pathogenic agents can enter the bloodstream through microcracks in your skin. If the tick has already sucked in, you should remove it as quickly as possible to reduce the risk of infection. There are special tools for removing ticks, which look like a small nail puller (a “spoon” with a slot) for picking up the tick and removing it by rotation. One can easily DIY such a tool from a piece of a plastic bottle.
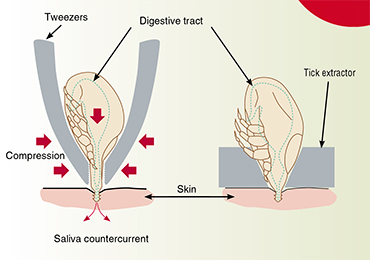 You can also remove the tick with pointed-end tweezers by pinching it as close to the skin as possible. Pull the tick cautiously so as not to damage the mouth parts. You can also remove the tick using a thread loop tightened on the tick’s head as close to the skin as possible. You should pull the thread gradually, twisting it in one direction. If the tick has bitten you in an inconvenient place and there is no one can to help you, then remove it in any way possible, even if you damage its integument.
You can also remove the tick with pointed-end tweezers by pinching it as close to the skin as possible. Pull the tick cautiously so as not to damage the mouth parts. You can also remove the tick using a thread loop tightened on the tick’s head as close to the skin as possible. You should pull the thread gradually, twisting it in one direction. If the tick has bitten you in an inconvenient place and there is no one can to help you, then remove it in any way possible, even if you damage its integument.
When a tick has been removed carefully, parts of its oral apparatus rarely remain in the skin, but sometimes this may happen. This will not affect the likelihood of disease, but the remains of the tick can cause irritation and inflammation at the bite site. Therefore, it is better to remove them immediately, as is done with ordinary splinters, and disinfect the area with alcohol or another disinfectant (you may also rub an antibiotic ointment into the bite site). If you subsequently develop symptoms of a secondary infection, as with a splinter, you should see a doctor.
The probability of disease after a tick bite depends on many factors. For example, on how long the tick has been on the body, on how infected the tick itself was, and on how the person’s immune system works. There is an opinion that it takes up to 48 hours to transmit Lyme disease pathogens from a tick to a human, so international recommendations discourage testing the tick if it has sucked for less than 36 hours. Still, although the probability of infection is really small, it is not zero. Practice shows that a person can contract infection even after a short-term suction.
ECOLOGICAL CONTROL OF TICKS Ixodid ticks have few natural enemies that could be used as agents of biological control of tick populations. American researchers showed that in several geographically isolated areas of New England, where there are many deer and blacklegged ticks (close relatives of our taiga ticks), the latter are attacked by the parasitic wasp Ixodiphagus hookeri (Renjie, Hyland, and Oliver, 1998). However, its overall impact on the tick population, as well as on other small arthropod predators and birds, is low. When blacklegged tick females suck blood, they can be infected by some types of parasitic roundworms (nematodes), but nematodes do not tolerate the low temperatures typical of our climate.
American researchers showed that in several geographically isolated areas of New England, where there are many deer and blacklegged ticks (close relatives of our taiga ticks), the latter are attacked by the parasitic wasp Ixodiphagus hookeri (Renjie, Hyland, and Oliver, 1998). However, its overall impact on the tick population, as well as on other small arthropod predators and birds, is low. When blacklegged tick females suck blood, they can be infected by some types of parasitic roundworms (nematodes), but nematodes do not tolerate the low temperatures typical of our climate.
Pathogenic fungi, such as Beauveria bassiana and Metarhizium anisopliae, are considered more promising agents, with proven efficacy against blacklegged ticks when applied on the border of residential areas (Greeshma Rao UB and Narladkar, 2018).
M. anisopliae is a soil fungus that can infect insects and ticks. The fungus spores attach to the surface of the host and germinate inward, forming filamentous mycelium and releasing toxins. One of the strains of this fungus became the basis for a biopesticide agent against ticks, which is developed by the company Novozymes Biologicals Inc. (United States). Tests were conducted in 2007 in Connecticut and New Jersey to show that the product can be used to control the population of blacklegged tick nymphs. The company is developing a granular anti-tick product containing spores of this fungus. A good thing about the new product is its minimal activity against nontarget organisms; it does no harm to beneficial insects such as honey bees and earthworms.
The invention of effective genetic technologies opened up new possibilities for influencing the primary reservoir of tick-borne infections. Thus, scientists from the Massachusetts Institute of Technology proposed to use gene drive (certain genes that are specially programmed for a quick spread in the animal population) in a project called Mice Against Ticks (Buchthal et al., 2019). In the United States, larvae and nymphs feed mostly on white-footed mice. Scientists proposed to edit their genome by introducing a gene for ongoing synthesis of antibodies that inactivate Lyme disease (tick-borne borreliosis) pathogens. This gene is integrated into a construct that ensures its transmission to all the progeny of the genetically modified mouse. The cross-breeding of these mice with their wild fellows should soon create a situation whereby almost all animals in the population are carriers of this gene. Borrelia will not survive in the organisms of these mice, and the infection reservoir will disappear or diminish significantly, leading to a decrease in tick-borne infection
It is advisable to take the removed tick to a laboratory for research. The tick must be either alive (in this case, it is placed in a closed container or plastic bag with a piece of wet cotton or forest greens and stored in the refrigerator) or frozen.
In Russia, all specialized laboratories examine ticks by PCR for RNA of the tick-borne encephalitis virus and DNA of the Lyme disease pathogen. Some laboratories also test for DNA of causative agents of rickettsioses and other rarer diseases (granulocytic anaplasmosis and monocytic ehrlichiosis).
However, even if the tick test shows the presence of an infectious agent, this does not mean that the bitten person will necessarily contract this infection. One way or another, you should carefully monitor the state of your health for one month after the tick bite and, if possible, avoid going to places where you may not get medical care.
If the tests for tick-borne encephalitis and Lyme disease are negative, but you have a fever or other flu-like symptoms, you should consult an infectious disease specialist. These symptoms may manifest the onset of another tick-borne infection or arise as a result of another tick bite that went unnoticed. In any case, if you spend spring and summer in regions with a high risk of infection, you should pay special attention to your general health.
As concerns preventive antibiotic treatment after tick bites, here opinions differ. As a rule, health practitioners in the United States and in most European countries do not recommend it. In 2019, the Infectious Diseases Society of America proposed that preventive antibiotic therapy of Lyme disease be carried out only at a high risk of infection, if the case has occurred in a region of high incidence of tick-borne borreliosis and the sucking tick has remained on the body for more than 36 hours. If the patient develops manifestations of migratory erythema, he or she then receives a standard course of antibiotic therapy.
CHIMERIC ANTIBODIES AGAINST TICK-BORNE ENCEPHALITIS VIRUS To date, there is no effective treatment for tick-borne encephalitis. People bitten by ticks receive anti-tick immunoglobulin for treatment and for emergency prevention. These protective proteins (antibodies) are obtained from the serum of donors who are immune to the encephalitis virus. In Russia, immunoglobulin therapeutics are manufactured by NPO Virion (the Tomsk branch of NPO Mikrogen) and by some blood transfusion stations.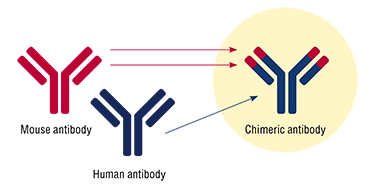 Serum-based immunoglobulin products demonstrate a moderate therapeutic effect; however, they have a series of disadvantages. Firstly, due to the low content of anti-tick antibodies in the donor blood, patients receive relatively high doses of the foreign protein material, with many nontarget antibodies and other protein molecules simultaneously entering their bodies. This can cause allergic reactions and other side effects.
Serum-based immunoglobulin products demonstrate a moderate therapeutic effect; however, they have a series of disadvantages. Firstly, due to the low content of anti-tick antibodies in the donor blood, patients receive relatively high doses of the foreign protein material, with many nontarget antibodies and other protein molecules simultaneously entering their bodies. This can cause allergic reactions and other side effects.
Secondly, due to technological difficulties, it is virtually impossible to produce standardized batches of serum-based immunoglobulins in which the concentration ratios of total protein and protective antibodies would not vary from batch to batch. Finally, the use of any drugs based on donor blood is always associated with risk because blood is currently tested only for the presence of HIV and hepatitis B and C viruses whereas researchers have been discovering more and more of viral pathogens in recent years.
The situation in Russia justifies the use of serum-based immunoglobulin products because ticks in Siberia and the Far East carry especially dangerous strains of tick-borne encephalitis virus. Anti-tick immunoglobulin can prevent the development of a severe, possibly lethal, form of this disease. In European countries, where the causative agent of tick-borne encephalitis is the European subtype of the virus, the disease takes a mild course. Patients usually receive only symptomatic, supportive therapy; therefore, these countries were able to abandon the production and use of the drug based on donated blood.
Not surprisingly, it was Russian scientists who came up with the idea of a technology for the production of “pure” antibodies that neutralize tick-borne encephalitis virus without using donor or animal blood components.
At first glance, the idea of creating drugs based on full-sized antibodies, i. e., the molecules that vertebrate organisms have long and successfully used to combat pathogens, seems easy to realize. In recent decades, dozens of highly effective drugs of a new generation have been developed, mainly for the treatment of cancer and autoimmune diseases. However, it was only in the very recent years that technologies appeared that allow almost guaranteed production of recombinant (hybrid) human antibodies against various infectious agents.
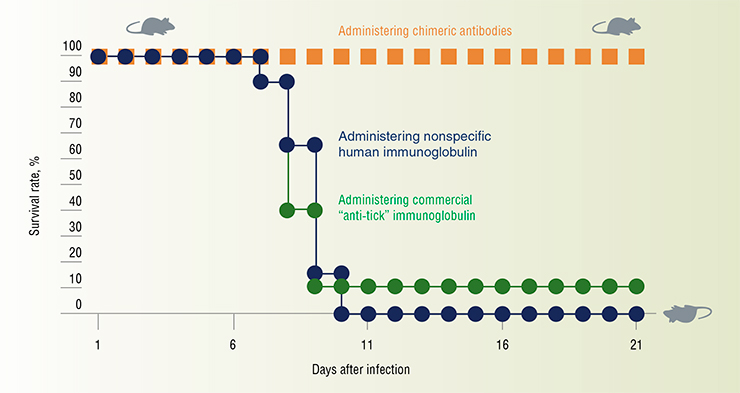
These technologies were used by scientists at the Institute of Chemical Biology and Fundamental Medicine SB RAS (Novosibirsk) to develop a chimeric antibody against tick-borne encephalitis virus. It is a human immunoglobulin with a built-in fragment of a mouse antibody that tightly binds the viral particle. The share of the human part of the molecule is more than 96 %.
Preclinical trials have been completed successfully. Experiments on laboratory animals showed that the introduction of recombinant antibodies can provide effective protection against hundreds of lethal doses of tick-borne encephalitis virus. To date, a stable CHO strain (one of the most common mammalian cell lines in the pharmaceutical industry, which originates from Chinese hamster ovary cells) has been obtained, which produces a new anti-tick antibody, and methods have been developed for purifying this antibody. The next step is to conduct clinical trials and organize production
Russian doctors recommend a preventive course of antibiotics if the tick is found to carry borrelia. Importantly, up to a half of ixodid ticks in Siberia may be carriers of these pathogens, and borrelioses relatively often take a nonerythemous form, which complicates the diagnosis. Perhaps, it is the different approach to the preventive use of antibiotics that explains the significantly lower number of cases of chronic Lyme disease in Russia, compared with Europe, where treatment begins only after a confirmation of the diagnosis. For many diseases, early treatment increases the chances of cure.
 In each particular case, many factors must be taken into account. It hardly makes sense to carry out preventive antibiotic therapy for a young hunter, whom ticks bite almost every day. But this therapy might be medically necessary for an elderly patient with a weakened immune system, who has been bitten by a tick for the first time. Special attention should be paid to children, who need medical supervision after a tick bite, and the therapist must make a decision taking into account all factors.
In each particular case, many factors must be taken into account. It hardly makes sense to carry out preventive antibiotic therapy for a young hunter, whom ticks bite almost every day. But this therapy might be medically necessary for an elderly patient with a weakened immune system, who has been bitten by a tick for the first time. Special attention should be paid to children, who need medical supervision after a tick bite, and the therapist must make a decision taking into account all factors.
Pets should also be protected against ticks and tick-borne infections. It is dogs who come into contact with ticks most often, even despite the vigorous preventive measures, including the use of sprays and anti-tick collars impregnated with acaricides. Dogs can develop Lyme disease; in the European part of Russia and in the south of Western Siberia, the most serious dog disease is pyroplasmosis (or babesiosis) (Cassio et al., 2002; Rar et al., 2005).
In the absence of treatment, this disease is almost always lethal, and measures to save the animal must be taken immediately. If you find a sucking tick on a dog, you should observe its health condition after the bite. The incubation period of pyroplasmosis lasts from one day to three weeks. If the dog becomes lethargic and reluctant to move; if it refuses to take walks and stops eating; if its body temperature rises above 39.5 °C—all these signs are a cause for alarm even if you did not notice a tick bite. In the absence or delayed treatment, the dog grows weaker every day, and it may develop hind limb paralysis and other serious disorders.
The most reliable way to avoid tick-borne encephalitis is timely vaccination. The first tick-borne encephalitis vaccine was developed in the Soviet Union almost immediately after the discovery of this virus in 1937. It was a formaldehyde-inactivated suspension of the brains of mice infected with the virus strain Sofjin, which was isolated from the brain of a patient who died from tick-borne encephalitis in the Far East. In 1939, clinical trials of the first anti-tick vaccine were successfully completed, proving its high efficacy. During the development of this vaccine, the virologist N.V. Kagan and laboratory assistant N. Utkina contracted tick-borne encephalitis and died.In 1958, a modified version of this vaccine came into use in the Soviet Union, in all the regions with reported incidence of tick-borne encephalitis. By the end of the 1980s, researchers developed an anti-tick vaccine based on a highly purified concentrated Sofjin virus produced in a cell culture. Since that time, tens of millions of doses have been produced in the Soviet Union, and then in the Russian Federation.
Three vaccines are currently produced in Russia: “Tick-borne encephalitis vaccine, culture-based, purified, concentrated, inactivated, dry,” Kleshch-E-Vak, and Entsevir. All the Russian vaccines reliably protect against contracting tick-borne encephalitis; there are versions of these vaccines for children from an early age.
The first European anti-tick vaccine FSME-Immun was developed in 1976. In 1991, the second European anti-tick vaccine Encepur was registered in Germany. Both vaccines are based on the inactivated tick-borne encephalitis virus belonging to the European subtype, which usually causes only mild forms of the disease
Pyroplasmosis is diagnosed by microscopic detection of babesias in blood smears. The most effective drug is imidocarb, and in the case of delayed diagnosis, it is supplemented by a course of doxycycline antibiotics. Unfortunately, dogs do not develop persistent immunity to pyroplasmosis and may contract this disease again within one season. Now there are several different pyroplasmosis vaccines, which do not provide full protection yet reduce the number of deaths in animals.
If you prefer an active lifestyle and spend much time in nature for leisure or because of your professional occupation, you should know that today nothing provides 100 % protection against ixodid ticks and tick-borne infections in regions that are epidemiologically unsafe. However, you can significantly reduce the likelihood of a tick bite if you follow several simple rules.

If you failed to avoid a tick attack, the most important thing is not to panic! And not to waste time: the sooner you remove the tick and deliver it for analysis for the presence of pathogens dangerous to humans, the sooner you can begin—if necessary—emergency prevention or therapy. Moreover, do not forget that vaccination against tick-borne encephalitis is the only reliable way to protect against this most dangerous tick-borne virus infection in Russia.
Armed with knowledge, we can minimize the likelihood of encounters with ixodid ticks and increase our chances of staying healthy even if we cannot avoid tick attacks.
References
Vlasov V. V., Tikunova N. V. Chronic Lyme disease: nonexistent illness or wrong diagnosis? // SCIENCE First Hand. 2019. V. 53. N 3. P. 32–41.
Korenberg E. I., Pomelova V. G., Osin N. S. Prirodnoochagovye infektsii, peredayushchiesya iksodovymi kleshchami (Zoonotic Infections Transmitted by Ixodid Ticks). Moscow, 2013 [in Russian].
Rudakov N.V. Rikketsii i rikketsiozy. Rukovodstvo dlya vrachei (Rickettsia and Rickettsioses. Guidelines for Doctors). Omsk: Omskii Nauchnyi Vestnik, 2016 [in Russian].
Somova L. M., Frolova M. P., Pogodina V. V., Leonova G. N. Patologiya neiroinfektsii, vyzyvaemykh virusami kompleksa kleshchevogo entsefalita (monografiya-atlas) (Pathology of Neuroinfections Caused by Tick-Borne Encephalitis Viruses (Monograph & Atlas)). Moscow: Sinteriya, 2018 [in Russian].
Carr A. L., Salgado V. L. Ticks home in on body heat: A new understanding of Haller's organ and repellent action // PLoS One. 2019. V. 14(8). P. e0221659. doi: 10.1371/journal.pone.0221659.
Caccio S. M., Antunovi B., Moretti A., et al. Molecular characterisation of Babesia canis canis and Babesia canis vogeli from naturally infected European dogs // Vet. Parasitol. 2002. V. 106. P. 285–292.
Igolkina Y., Krasnova E., Rar V., et al. Detection of causative agents of tick-borne rickettsioses in Western Siberia, Russia: identification of Rickettsia raoultii and Rickettsia sibirica DNA in clinical samples // Clin. Microbiol. Infect. 2018a. V. 24(2). P. 199.e9–199.e12.
Mediannikov O. Y., Sidelnikov Y., Ivanov L., et al. Acute tick-borne rickettsiosis caused by Rickettsia heilongjiangensis in Russian Far East // Emerg. Infect. Dis. 2004. V. 10(5). P. 810–817.
Platonov A. E., Karan L. S., Kolyasnikova N. M., et al. Humans infected with relapsing fever spirochete Borrelia miyamotoi, Russia // Emerg. Infect. Dis. 2011. V. 17(10). P. 1816–1823.
Rar V. A., Maksimova T. G., Zakharenko L. P., et al. Babesia DNA detection in canine blood and Dermacentor reticulatus ticks in southwestern Siberia, Russia // Vector Borne Zoonotic Dis. 2005. V. 5(3). P. 285–287.














